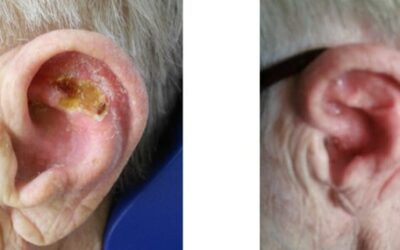
Knee bone marrow edema is often diagnosed with the help of MRI as a consequence of trauma, overload, surgery, arthrosis or osteonecrosis. One of its most common reasons is cruciate ligament rupture surgery. The edema pathogenesis is not known for sure. The bone marrow edema is associated with stressful pain and may also contribute to increased arthrosis formation due to improper loading of the knee. Since this thesis is not proven, the pain treatment is in the foreground. Standard therapy is knee load relief (using crutches), physiotherapy, ilomedin infusions and surgical treatment of the edema. A therapeutic response can be achieved in about 70% of cases. Bone marrow edema can occur in the femoral condyles as well as in the tibial head and differ in localization and extent.
In their study “Radiotherapy Treatment For Post Traumatic Knee Bone Marrow Edema” Franz Böhler, Valerio d’Arrigo, Patrick Clemens, Raoul Pinter, Robert Tetickovic, Alexander DeVries, investigated possible radiotherapy treatments for post traumatic knee bone marrow edemas.
Patient data was evaluated prospectively before and after radiotherapy using an Xstrahl 200 as well as during the 6 to 8-week control under standard conditions, also in the case of a second or third irradiation series (RTZ-Series). Referrals for 7 patients with 9 treatment-resistant bone marrow edema to be treated during this timeframe. All cases resulted from a trauma: 3 – slight trauma, 3 – had tried physiotherapy and load relief for trauma treatment, 2 had had edema surgical treatment. The median age at the beginning of the therapy was 58 years (45 – 72).
The treatment was done by 2 opposite fields in single doses of 1 Gy (4 knees), with 0.5 Gy (5 knees) and a total dose of 6 or 3 Gy.
At the end of the first RTX-series, there were 3 CR, 5 PR and 1 SD (33/56/11%), at 6-week control – 4 CR, 2 PR, but also 2 PD (22%), where a patient with PD had an imaging CR according to MRI and thus the persistent pain might be of a different origin. A second RTX-series was performed on 4 knees (44%), further improvement was achieved in 3 cases, but for the patient with SD there was not any relief achieved after the third RTX-series. Pain intensity as per VAS was reduced from an average of 5.4 to 1.9 after the first RTX-series, from 4.3 to 2 after the second RTX series. The final result was 5 CR, 3 PR and only one SD (56 / 33/11%), corresponding to a response rate of 89%.
Therefore, it was concluded that a low-dose radiotherapy of the bone marrow edema of the knee is an efficient treatment method. But perspective data under study conditions are still pending.
This Xstrahl In Action was adapted from a article found on a National Library of Medicine website.